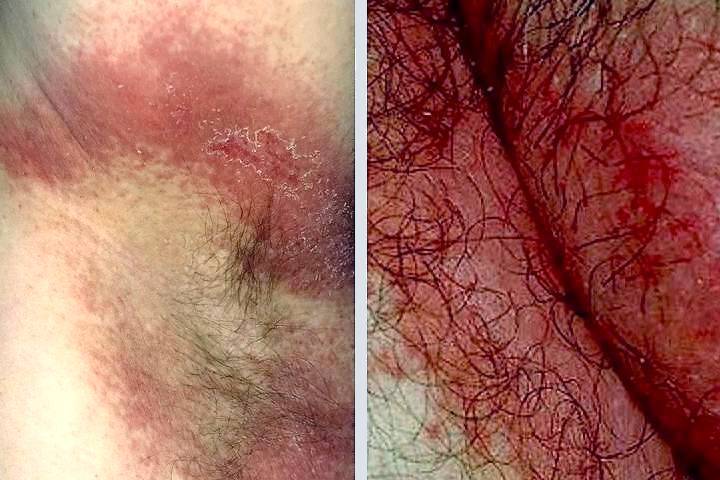
Groin rashes are often misdiagnosed, leading to ineffective treatments and prolonged discomfort; seeking a specialist dermatologist ensures accurate identification and targeted care.
Key Areas We Will Cover
-
Common types of groin rashes, including fungal, bacterial, and inflammatory conditions
-
Causes and symptoms specific to men, influenced by lifestyle and physiology
-
The critical role of professional dermatological diagnosis
-
Effective treatment options tailored to each rash type
-
Preventive measures and daily habits to minimise recurrence
-
Why The Skin Care Network stands out for men’s dermatology in London
-
How to book your consultation for personalised care
Introduction
Groin rashes in men are a prevalent concern in the UK, often arising from sweat, friction, heat, or infections, and exacerbated by active lifestyles or occupational demands. These conditions can cause significant discomfort, itching, and embarrassment, impacting daily life and confidence. This comprehensive guide delves into groin rash treatment for men in London, highlighting the importance of proper diagnosis to differentiate between various causes, from fungal infections to eczema. At The Skin Care Network, our expert dermatologists provide personalised solutions, ensuring effective management and long-term skin health.
Understanding Groin Rashes in Men
Groin rashes encompass a range of skin conditions affecting the inner thighs, genitals, and surrounding areas. They are particularly common in men due to higher sweat production, hair density, and friction from activities like exercise or manual work.
Why Men Are More Susceptible
Men’s skin in the groin area faces unique challenges: thicker skin layers, increased sebum production, and frequent exposure to moisture from sports or tight clothing. Factors such as obesity, diabetes, or weakened immunity can heighten risks, with lifetime prevalence of fungal groin infections estimated at 10 to 20%.
Common Types of Groin Rashes
Accurate identification is essential, as symptoms can overlap. Below, we outline key conditions based on expert insights.
Fungal Infections
-
Groin Tinea (Tinea Cruris or Jock Itch): Caused by fungi like Trichophyton rubrum, thriving in warm, moist environments. Common in athletes, it presents as a red, scaly rash with a defined border, often itchy and spreading to thighs.
-
Groin Candida (Candidiasis): A yeast infection from Candida species, leading to red, moist patches with satellite pustules. It flourishes in humid conditions and can coexist with bacterial issues.
Bacterial Infections
-
Groin Erythrasma: Triggered by Corynebacterium minutissimum, appearing as pink or brown patches with fine scaling. It mimics fungal rashes but requires antibacterial treatment.
-
Folliculitis in the Groin: Inflammation of hair follicles, often bacterial (e.g., Staphylococcus), resulting in red, pus-filled bumps. Shaving or friction exacerbates it.
Frictional and Sweat-Related Rashes
-
Frictional Rash (Intertrigo): Skin-on-skin rubbing in folds causes inflammation, worsened by moisture. Secondary infections with bacteria or fungi are common.
-
Sweat Rashes (Miliaria) in the Groin: Blocked sweat ducts from heat and exercise lead to itchy bumps or blisters, particularly in flexures during hot weather.
Other Inflammatory Conditions
-
Male Groin Acne: Clogged pores cause acne-like eruptions, influenced by sebum and friction.
-
Hidradenitis Suppurativa: A chronic condition with painful boils and abscesses in sweat glands, often requiring specialist management.
-
Eczema (Atopic, Allergic, or Irritant): Itchy, red patches from genetic factors, allergens, or irritants like soaps.
-
Psoriasis: Scaly plaques, sometimes inverse in folds, causing discomfort without typical scales.
Rare but Serious Presentations
Rarely, persistent groin rashes may indicate skin cancers like Bowen’s disease (squamous cell carcinoma in situ) or Paget’s disease, presenting as fixed, non-healing lesions. Early detection is vital.
Recognising Symptoms
Symptoms often include itching, redness, scaling, blisters, or pain. Men may experience worsening after sweating, with odours in infected cases. Persistent or severe signs warrant professional evaluation to rule out complications.
The Importance of Proper Dermatological Diagnosis
Self-treatment can worsen conditions, such as using steroids on fungal or bacterial rashes, leading to resistance or spread. Our dermatologists use thorough examinations, skin swabs, or advanced tools like confocal laser microscopy for precise diagnosis without invasive procedures. This ensures treatments target the root cause, avoiding confusion between similar presentations like sweat rashes and polymorphic light eruption.
Effective Treatment Options
Treatments vary by cause and are prescribed after diagnosis.
Topical Therapies
-
Antifungal creams (e.g., miconazole) for tinea or candida often clear in 1 to 3 weeks.
-
Antibacterial agents for erythrasma or folliculitis.
-
Mild topical steroids for inflammatory conditions like miliaria or eczema, used short-term to reduce redness.
-
Combined preparations (e.g., antifungal with hydrocortisone) for intertrigo with secondary infection.
Advanced Interventions
For chronic cases like hidradenitis, options include oral antibiotics or biologics. Laser hair removal may help in grooming-related folliculitis
Managing Mixed Infections
Rashes with bacterial, fungal, or candidal elements require tailored combinations, avoiding steroids alone to prevent exacerbation.
Preventive Measures and Lifestyle Tips
Prevention focuses on hygiene and habits:
-
Wear loose, breathable cotton underwear to reduce friction and moisture.
-
Shower promptly after exercise, drying thoroughly (use a cool hairdryer if needed).
-
Maintain a healthy weight and manage underlying conditions like diabetes.
-
Use fragrance-free, gentle cleansers; avoid harsh soaps.
-
Change clothes daily and launder in hot water.
Why Choose The Skin Care Network?
Our London clinic excels in men’s dermatology, with GMC-registered specialists offering discreet, flexible appointments. We use cutting-edge diagnostics for rapid results, boasting a 90% patient satisfaction rate. Unlike lengthy NHS waits, we provide same-day assessments and personalised plans.
Conclusion
Groin rashes in men, from fungal infections to eczema, can be debilitating but are manageable with expert care. Key takeaways include recognising diverse causes, prioritising diagnosis to avoid misuse of treatments like steroids, and adopting preventive routines. At The Skin Care Network, we empower men to regain comfort and confidence through targeted therapies.
Ready to Resolve Your Groin Rash?
Take the first step towards relief. Book your consultation at The Skin Care Network today. Call 0208 441 1043 or click ‘Make an Appointment’ for expert, male-focused dermatology care. Do not let discomfort linger; get the diagnosis and treatment you deserve.
Frequently Asked Questions About Groin Rash Treatment
Groin rashes can stem from various causes, making self-diagnosis challenging. Below, we answer common queries to guide you towards informed decisions and effective care at The Skin Care Network.
Heat, sweat, friction, fungal or bacterial infections, and inflammatory conditions like eczema are primary triggers, often worsened by active lifestyles.
If symptoms persist beyond a week, worsen with over-the-counter remedies, or involve pain, swelling, or discharge, consult a dermatologist for an accurate diagnosis.
Yes, our tailored approaches, such as antifungal creams or mild steroids, are safe when prescribed correctly, considering men’s thicker skin and higher sweat rates.
Absolutely, through good hygiene, breathable clothing, and prompt drying after sweating, recurrence can be significantly reduced.
Expect a 15 to 30 -minute session with a skin examination, history review, possible tests, and a customised treatment plan, often with immediate insights.



