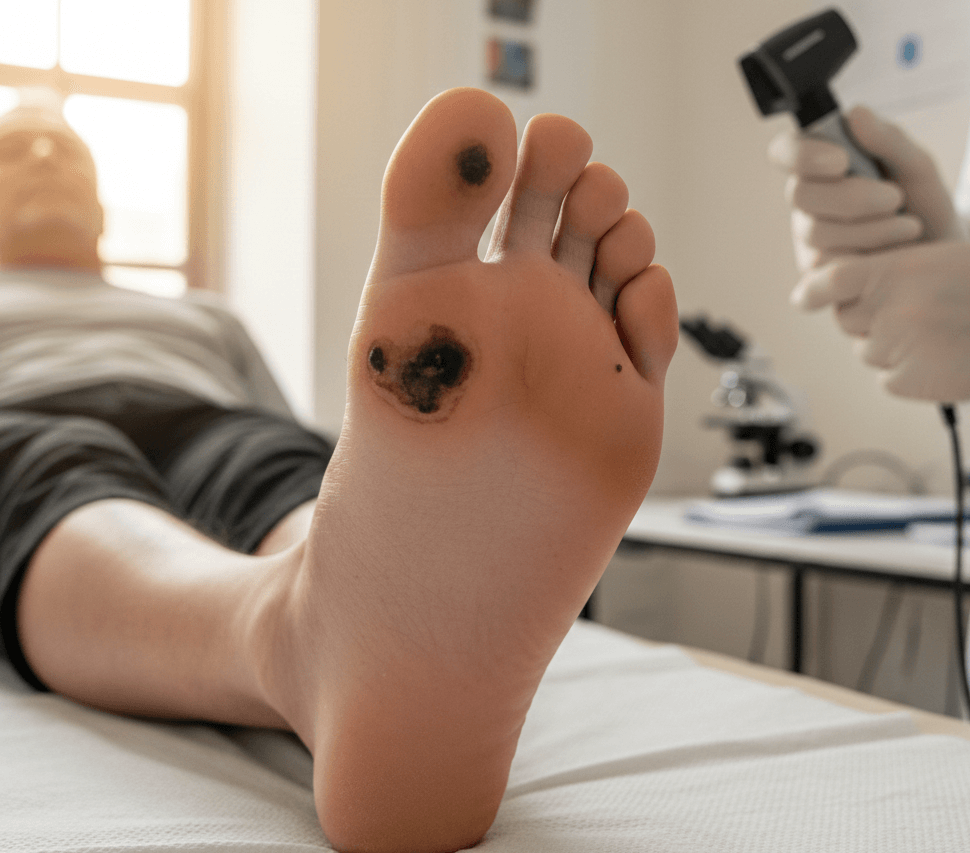
Did you know that acral melanoma, a rare but aggressive skin cancer on the palms, soles, or under nails, shows distinct risk patterns unlike sun-related melanomas? A groundbreaking 2026 study in JAMA Dermatology on US veterans has identified Agent Orange exposure as a key factor increasing odds, alongside female sex, certain ethnicities, and prior skin lesions, challenging traditional assumptions and urging better awareness in the UK, where delayed diagnosis remains a concern.
Key Areas We Will Cover
- What acral melanoma is and why it differs from common melanomas.
- Breakthrough risk factors from the latest US veterans study.
- How these findings apply to UK patients, including ethnic diversity and non-UV causes.
- Signs, early detection challenges, and prevention strategies.
- Why professional checks matter, especially for high-risk groups.
- When to seek specialist care in London and Hertfordshire.
Introduction
Acral melanoma, often called acral lentiginous melanoma, is a rare subtype of skin cancer that develops in sun-protected areas like the palms, soles, or nail beds. While dermatologists’ expertise traditionally focuses on UV-driven melanomas, emerging research highlights unique risks for acral types. A recent US study on veterans reveals environmental and clinical factors that could inform UK care, where acral cases are less common in fair skin but more prevalent in darker tones and often diagnosed late. At The Skin Care Network, our dermatologist team in Barnet translates global breakthroughs into practical guidance for early intervention and better outcomes.
What Is Acral Melanoma and Why Is It Different?
Acral melanoma arises from melanocytes in thick-skinned, non-sun-exposed areas. Unlike superficial spreading melanoma (linked to UV damage), it shows minimal UV signature and affects all skin types, though it predominates in people with darker skin in the UK and globally.
- Accounts for 2-3% of melanomas in White populations but up to 35-60% in darker skin tones.
- Often presents later, contributing to higher morbidity.
- Not strongly tied to sunbeds, sunburns, or cumulative UV exposure.
Breakthrough Insights: Risk Factors from the US Veterans Study
The 2026 JAMA Dermatology case-control study analysed US veterans, identifying:
- Agent Orange exposure is linked to higher odds of acral melanoma (a herbicide used in Vietnam, relevant for older veterans, but highlighting environmental toxins).
- Increased risk in females, certain races/ethnicities (e.g., higher in non-White groups), and those with prior skin lesions.
- Reduced odds in some groups, suggesting protective or differing factors.
These findings underscore acral melanoma’s distinct biology, separate from UV-centric risks in most UK cases.
Applying US Findings to UK Patients
In the UK, acral melanoma remains rare overall, with no direct Agent Orange equivalent, but parallels exist:
- Potential trauma or mechanical stress (e.g., friction on feet) is a debated trigger, seen in weight-bearing sites.
- Genetic factors under study, with no strong familial links yet.
- Higher relative incidence in ethnic minorities with darker skin, where public awareness of non-sun melanomas is lower.
- Overlapping with general melanoma trends: Stabilising incidence in younger groups, but persistent challenges in older or diverse populations.
Our Barnet clinic sees varied cases, emphasising inclusive screening.
Signs to Watch For and Early Detection
Look for:
- Dark streaks under nails (subungual).
- Irregular pigmented patches on palms/soles.
- Changing or asymmetric lesions that evolve.
Use the ABCDE rule, but adapt for acral: Focus on evolution, as borders/colours differ. Self-checks help, but professional dermoscopy is essential due to subtle early signs.
Prevention and Management Strategies
- Regular skin checks, including palms, soles, and nails, especially if higher risk (darker skin, history of lesions, older age).
- No strong UV link, so focus on overall skin health: Moisturise to reduce friction, avoid trauma.
- Prompt biopsy for suspicious changes improves prognosis.
Conclusion
Acral melanoma’s unique risk profile, highlighted by the US veterans study, reminds us that not all skin cancers follow the sun-exposure rule. Early recognition of subtle changes in non-exposed areas can prevent advanced disease. Combining global research with UK realities empowers better protection for diverse patients.
Take Control of Your Skin Health with The Skin Care Network Today
Concerned about unusual pigmentation on your hands, feet, or nails? Our experienced dermatologist team offers expert, discreet assessments.
📍 Visit us at 68-70 Union St, Barnet EN5 4HZ, United Kingdom
📞 Call +44 20 8441 1043 to book your consultation. Early action makes all the difference. Schedule today.
Frequently Asked Questions
Addressing common concerns helps readers feel informed and proactive about acral melanoma risks.
It develops in sun-protected areas and has weaker ties to UV exposure, often linked to other factors like trauma or genetics.
Yes, relatively higher in people with darker skin tones, though overall rare.
Not directly (no widespread exposure), but it highlights how environmental factors can influence rare subtypes beyond UV.
Examine palms, soles, and nails monthly for new/dark streaks or patches; seek a dermatologist for any concerns.
If you notice evolving lesions in these areas, especially with risk factors like darker skin or prior changes, don’t delay professional evaluation.