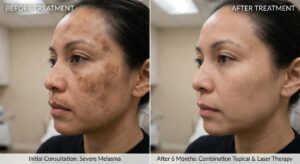
Melasma Treatment Advances: Exploring the Latest Topical Options in 2026
“Every year brings more promising topical choices for melasma, giving us valuable new tools to help patients achieve clearer, more even-toned skin.”
Melasma remains one of the most challenging forms of facial hyperpigmentation, often triggered by sun exposure, hormones, and genetics. At The Skin Care Network, our dermatologist team closely follows the latest developments to deliver safe, effective, and personalised regimens for patients across the UK.
Key Areas We Will Cover
- The continued role of traditional first-line topical therapies
- Azelaic acid: A well-tolerated multi-action agent
- Kojic acid and tranexamic acid: Effective in supportive roles
- Cysteamine: A reliable antioxidant option with practical considerations
- 2-MNG (Melasyl™) and malassezin: Innovative agents with strong clinical data
- Thiamidol: A standout tyrosinase inhibitor delivering visible results
- The importance of combination approaches and emerging agents
- Practical guidance for UK patients seeking professional melasma care
What Role Do Traditional Topical Therapies Still Play in Melasma Management?
Traditional therapies, including hydroquinone, retinoids, steroids, and triple combination creams, continue to serve as reliable first-line options for many patients with melasma.
A long-established 2019 evidence-based review highlighted triple combination cream (hydroquinone, tretinoin, and a corticosteroid) and hydroquinone alone as highly effective when used appropriately under supervision. These agents work by suppressing melanin production, promoting cell turnover, and reducing inflammation.
While effective, they require careful monitoring to avoid potential side effects such as irritation or rebound pigmentation. At our Barnet clinic, we often begin with these proven treatments or integrate them thoughtfully with newer alternatives for improved long-term tolerability.
How Does Azelaic Acid Benefit Patients with Melasma?
Azelaic acid offers multifaceted relief through its anti-inflammatory, antioxidant, and anti-melanogenic properties, making it a favourite non-hydroquinone choice.
It not only helps lighten pigmentation but also calms redness, which is particularly helpful for sensitive or rosacea-prone skin. Clinical studies have shown favourable comparisons to 2% and 4% hydroquinone, with generally good patient tolerance. We commonly recommend azelaic acid as a standalone treatment or in layered regimens.
What Is the Role of Kojic Acid and Tranexamic Acid in Melasma Care?
Kojic acid works best within combination therapies, while tranexamic acid provides versatile support by targeting both melanin production and vascular factors.
Kojic acid contributes antimicrobial and pigment-inhibiting effects and is usually well tolerated. Tranexamic acid has gained significant attention in recent years; topical versions remain useful even though some studies suggest greater benefits from oral or injectable forms in select cases. Both ingredients enhance outcomes when combined with other actives.
Is Cysteamine a Suitable Option for Melasma?
Cysteamine functions as an antioxidant that reduces tyrosinase activity and inhibits melanogenesis, delivering helpful results for many individuals.
Meta-analyses and expert reviews support its efficacy and overall safety profile. Some patients note a distinctive odour, yet most find it tolerable and effective, with a 2023 consensus highlighting good patient acceptance despite occasional mild irritation, scaling, or dryness.
How Promising Are Newer Agents Like 2-MNG and Malassezin?
2-MNG (Melasyl™) and malassezin represent exciting innovations with unique mechanisms and favourable safety data.
Malassezin suppresses melanogenesis and has shown rapid responses in early research with minimal side effects; a small 2026 randomised trial demonstrated efficacy comparable to hydroquinone over 12 weeks.
2-MNG inhibits melanin synthesis downstream without directly blocking tyrosinase. 2025 studies found 0.5% 2-MNG non-inferior to 4% hydroquinone, with better tolerability, and similar performance to standard triple combination creams when paired with niacinamide. These ingredients are increasingly incorporated into daily sunscreens and moisturisers, offering broader accessibility.
Why Is Thiamidol Considered a Game-Changer for Melasma?
Thiamidol stands out as the most potent inhibitor of human tyrosinase identified to date, producing significant pigment reduction with excellent tolerability.
Multiple randomised trials and a 2023 systematic review confirm meaningful lightening within 12–24 weeks when applied at 0.1–0.2% two to four times daily. Patients often experience visible improvement with fewer side effects than traditional agents, and it performs well across various skin types. Recent real-world and comparative data continue to support its role as a valuable addition or alternative for maintenance therapy.
Why Are Combination Approaches Essential for Successful Melasma Treatment?
No single topical agent serves as a universal solution; combination strategies deliver the best outcomes for this persistent condition.
Dermatologists frequently layer compatible ingredients, always alongside rigorous daily broad-spectrum photoprotection. Emerging options such as methimazole, metformin, glutathione, and certain botanicals show early promise, though larger randomised trials are still needed for many. Botanicals in particular require cautious evaluation due to variable evidence quality.
How Can UK Patients Access Modern Melasma Treatment?
At The Skin Care Network, our experienced dermatologist conducts thorough assessments to create individualised plans that may include traditional therapies, newer agents such as thiamidol or 2-MNG, and supportive care. We focus on realistic expectations, consistent routines, and long-term maintenance to minimise recurrence.
Conclusion
Melasma treatment has advanced significantly in recent years, with a wider range of topical options offering effective and better-tolerated choices alongside established therapies. From azelaic acid and tranexamic acid to innovative ingredients like thiamidol and 2-MNG, patients now benefit from more personalised pathways. Consistent sun protection and professional oversight remain fundamental to lasting success.
Get Started Today
Ready to explore the latest topical options for melasma? Contact The Skin Care Network for a comprehensive consultation with our dermatologist. We will design a targeted regimen to help fade pigmentation and restore skin confidence.
Book your appointment now and take control of your skin health.📞 Call +44 20 8441 1043.
Frequently Asked Questions About Melasma Topical Treatments
Triple combination creams and hydroquinone remain highly effective first-line choices, but newer agents such as thiamidol and 2-MNG often match or exceed results with improved tolerability. A dermatologist’s assessment helps determine the optimal approach for your skin.
Yes. Azelaic acid, tranexamic acid, cysteamine, thiamidol, and 2-MNG provide effective pigment control with better safety profiles for extended use in many patients.
Visible changes often begin within 8–12 weeks, with more noticeable results after 12–24 weeks of consistent application combined with daily high-factor sunscreen.
Many, including thiamidol and 2-MNG, demonstrate good tolerability across phototypes in clinical studies. Professional evaluation ensures the safest and most suitable selection.
Absolutely. UV exposure can worsen melasma and undermine treatment progress, so broad-spectrum SPF 50+ daily use, along with physical barriers, is essential.